Teaching in courses:
Research Group
Personalized Health Technology

Group leader: Jakob E. Bardram
Personalized Health Technology is basic to creating the 21st-century healthcare delivery model, which is participatory, personalized, predictive, and preventive.
The Personalized Health Technology group researches technologies and methods that fosters a participatory, personalized, predictive, and preventive (P4) approach to healthcare. The overall vision is to shifts healthcare from a reactive, disease-centered approach to a proactive, individual-centered paradigm focused on chronic disease management and well-being. We apply "real-world" data and predictive models to forecast potential health issues, while using personalized technology to deliver preventive strategies aiming at mitigating these risks before they occur. Personalized care tailors treatments based on a patient's unique disease profile and lifestyle factors, and seeks to empowers patients as active partners in their own health management. We leverages digital technologies to maximize health outcomes and transform healthcare practices, moving towards a more effective and efficient system.
Research
The group's research is focused on what we call "Personalized Health Technology" [3], but this line of research has also been labeled as Pervasive Healthcare [1,2], Personal Health Informatics, Digital Health, Mobile Health (mHealth), or Health IoT (Internet-of-Things). These names overlap and more or less refer to the same. Our definition of personalized health technology is;
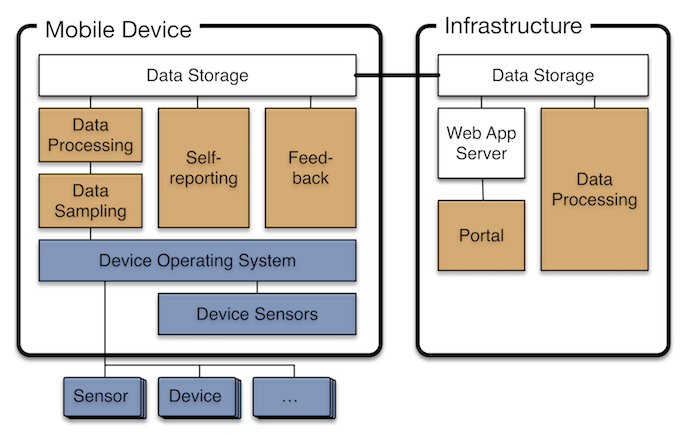
"...a generic class of pervasive computing technologies that uses personal mobile devices and back-end servers for health- and behavior-related data sampling, processing, visualization, and feedback." [3, p. 70]
A very generic software architecture for this kind of system is shown below (from [3]).
References
- Bardram, J. E. (2008). Pervasive healthcare as a scientific discipline. Methods of information in medicine, 47(03), 178-185.
- Arnrich, B., Mayora, O., Bardram, J., & Tröster, G. (2010). Pervasive healthcare. Methods of information in medicine, 49(01), 67-73.
- Bardram, J. E., & Frost, M. (2016). The Personal Health Technology Design Space. IEEE Pervasive Computing, 15(2), 70-78.
The group works in a set of core computer science research topics as well as in more health-application oriented research topics, including:
- Ubiquitous Computing, including Mobile and Wearable Sensing and Context-aware Computing
- Distributed Software Architectures for data collection, management, security, and privacy
- Feature Modelling and Machine Learning for behavior and disease modelling
- Human-Computer Interaction for the design of easy-to-use personal health technology
- Health-specific application development in psychiatry, neurology, diabetes, cardiovascular diseases, and cancer.
The group builds and maintains a set of software tools for its own and general use. Most of this is open-source and is available on GitHub. These tools include:
The Copenhagen Research Platform (CARP), which includes a wide range of software components, including:
- CARP Mobile Sensing – a mobile and wearable sensing framework for Flutter
- CARP Web Services – a cloud-based RESTful web service platform for collection, storage, and analysis of collected behavioural and health data.
- CARP Research Package – Flutter framework for informed consent and surveys.
- CARP Cognition Package – Flutter framework for cognitive tests.
CARP is available as a hosted service at DTU for researchers in Denmark to use for the collection of real-world patient data using the CARP Studies App, which is available from the app stores on Android and iOS.
All software components in CARP are available as open-source in our GitHub repositories, and all Flutter plugins and packages are available from pub.dev.
In addition, we maintain a set of open-source libraries for data collection and processing in the Digital Health GitHub repositories.
Ongoing research projects

The Internet-Based Cognitive Assessment Tool (ICAT) [1] is a web-based self-administered objective screening tool for remote testing of cognitive functioning. ICAT is implemented as a web application using the Copenhagen Research Platform for study management, participant management, and data storage. ICAT is an implementation of the paper-based Screen for Cognitive Impairment in Psychiatry (SCIP) assessment approach [2] and includes real-time assessment of verbal learning and recall using Automatic Speech Recognition (ASR) technology.
ICAT has been validated in a clinical study [3] which investigated whether ICAT is able to perform cognitive assessment in patients with Bipolar Disorder (BD) correctly as compared to the “golden standard” (the SCIP test). This was done by investigating (i) the sensitivity of ICAT to assess cognitive impairments, and (ii) the concurrent validity of the ICAT as compared to SCIP. Currently, more studies are ongoing.
This work is done in collaboration with the Department of Psychology at the University of Copenhagen and the Psychiatric Center, Copenhagen, in the Capital Region of Denmark.
References
- Hafiz, Pegah, Kamilla W. Miskowiak, Lars V. Kessing, Andreas Elleby Jespersen, Kia Obenhausen, Lorant Gulyas, Katarzyna Żukowska, and Jakob E. Bardram. The internet-based cognitive assessment tool: System design and feasibility study. JMIR formative research 3, no. 3 (2019): e13898.
- Miskowiak, K.W., Burdick, K.E., Martinez-Aran, A., Bonnin, C.M., Bowie, C.R., Carvalho, A.F., Gallagher, P., Lafer, B., Lopez-Jaramillo, C., Sumiyoshi, T., McIntyre, R.S., Schaffer, A., Porter, R.J., Purdon, S., Torres, I.J., Yatham, L.N., Young, A.H., Kessing, L.V., Vieta, E., 2018. Assessing and addressing cognitive impairment in bipolar disorder: the International Society for Bipolar Disorders Targeting Cognition Task Force recommendations for clinicians. Bipolar Disord. 20, 184–194.
- Miskowiak, K.W., Jespersen, A.E., Obenhausen, K., Hafiz, P., Hestbæk, E., Gulyas, L., Kessing, L.V. and Bardram, J.E., 2021. Internet-based cognitive assessment tool: Sensitivity and validity of a new online cognition screening tool for patients with bipolar disorder. Journal of Affective Disorders, 289, pp.125-134.

The Neuropathy Tracker [1] is a Mobile Health (mHealth) tool for ambulatory self-assessment of neuropathy, which can be done by the patient at home. The app was designed in an iterative user-centered design process involving neurologists, patients, and healthy subjects, thereby ensuring a high degree of clinical validity and usability. The assessment methodology in the app applies state-of-the-art neuropathy assessment methods and the app embodies a user-friendly and systematic assessment flow that guides the patient through the self-assessment.
The grading design of the Neuropathy Tracker includes the assessment of (i) general symptoms as a questionnaire, (ii) pin-prick sensation assessment, (iii) presence of allodynia or hyperalgesia, (iii) an assessment of large fiber sensation, (iv) motor examination, and (v) assessment of neuropathic pain.
The Neuropathy Tracker has been validated in a small feasibility study (N = 17), which showed a statistically significant concurrent validity when compared with a standard clinical assessment method. Further clinical validation studies are being conducted.
This research is done in collaboration with the University Hospital of Zealand in Roskilde and as part of the Greater Copenhagen Health Science Partners‘ Clinical Academic Group – the BAT-CAG.
References
- Bardram JE, Westermann M, Makulec JG, Ballegaard M (2025) The Neuropathy Tracker—A mobile health application for ambulatory and self-administred assessment of neuropathy. PLOS Digital Health 4(2): e0000725. https://doi.org/10.1371/journal.pdig.0000725

New technology for monitoring the heart rhythm of patients makes it possible for cardiologists at the hospital to cooperate with general practitioners (GPs) in new ways. This new model for treatment of cardiovascular diseases is called the "Cardio-Relay" for cross-sectional collaboration. Using this technology, GPs and cardiology patients are able to receive specialized advice from heart physicians without exhausting hospital visits. The CATCH project seeks to provide clinical evidence and commercial proof-of-concept for cross-sectoral ambulatory treatment using personal health technology. The project has a specific focus on heart failure (HF).
The CATCH project runs on the Copenhagen Research Platform and has been instrumental in the further design and development of the CARP Studies app for collection of physiological, contextual, and patient-reported data from patients in risk of HF. Based on this, we are identifying and developing digital biomarkers for early detection of HF and AF.
Group Leader
Jakob Eyvind Bardram Head of Sections, Professor Department of Health Technology Phone: +45 45256331 Mobile: +45 25550446 jakba@dtu.dk